HL7 FHIR Implementation Guide: Simplify Health Equity Application Reviews IG Release 1 - US Realm | STU1
0.1.0 - ci-build
HL7 FHIR Implementation Guide: Simplify Health Equity Application Reviews IG Release 1 - US Realm | STU1
0.1.0 - ci-build
HL7 FHIR Implementation Guide: Simplify Health Equity Application Reviews IG Release 1 - US Realm | STU1 - Local Development build (v0.1.0). See the Directory of published versions
The objective of the use case in this IG is to enable Community-Based Organizations (CBOs), social workers and providers to identify:
The use case has also been expanded to enable the presentation of Advance Directive details via the Patient Access API.
This Use Case leverages the following existing Implementation Guides with minor adaptations:
The SMART guides provide a mechanism to present the Digital Insurance Card IG content in a format that can be incorporated into a smartphones digital Wallet. The QR Code representation also suits itself to being carried as a traditional card, or even a printed paper document.
The SMART Health Links framework could also be extended to provide a QR Code link to an approved Prior Authorization. This would allow a patient to present the QR Code received from the prior authorization process as a form of payment to the service provider. The service provider can capture the information from the QR Code and use to submit a claim for the services rendered.
The Coverage Profile for the Digital Insurance Card has an extension added that links to Insurance Plan records stored in a Da Vinci Plan-Net Provider Directory:
The InsurancePlan profile in Da Vinci Plan-Net has an extension to link to a Questionnaire resource that is the Screening Assessment needed to determine if a beneficiary qualifies for the program or service:
These changes accomplish the following:
All of the above steps can be accomplished without requiring the CBO, Social Worker or Provider needing to login to the Health Plan. This approach dramatically simplifies the deployment of this use case.
This approach can also be integrated with the emerging Da Vinci Prior Authorization suite of IGs to enable streamlined authorization for Health Equity related programs or services.
The Coverage card can also have an extension that links to the PACIO ADI Goal, ADI Document Reference and a link to a member/patient’s Advance Directive resources. These data elements provide access to a Patient’s Advance Directive instructions:
SHEAR-AdvanceDirective-extension
The linkage of Advance Directive information with the Insurance Coverage record for a member increases the likelihood that a Patient’s wishes and instructions will be available to their Providers when needed.
The Digital Insurance Card provides the ability to create a QR code that can be scanned to link back to a Health Plan Member’s coverage, confirming valid coverage. This capability can also provide a linkage to a member’s Advance Directive instructions and wishes. The QR Code can be integrated into a smartphone wallet or can be printed, or included on a membership card. The use of a smartphone is not a requirement in this proposed implementation.
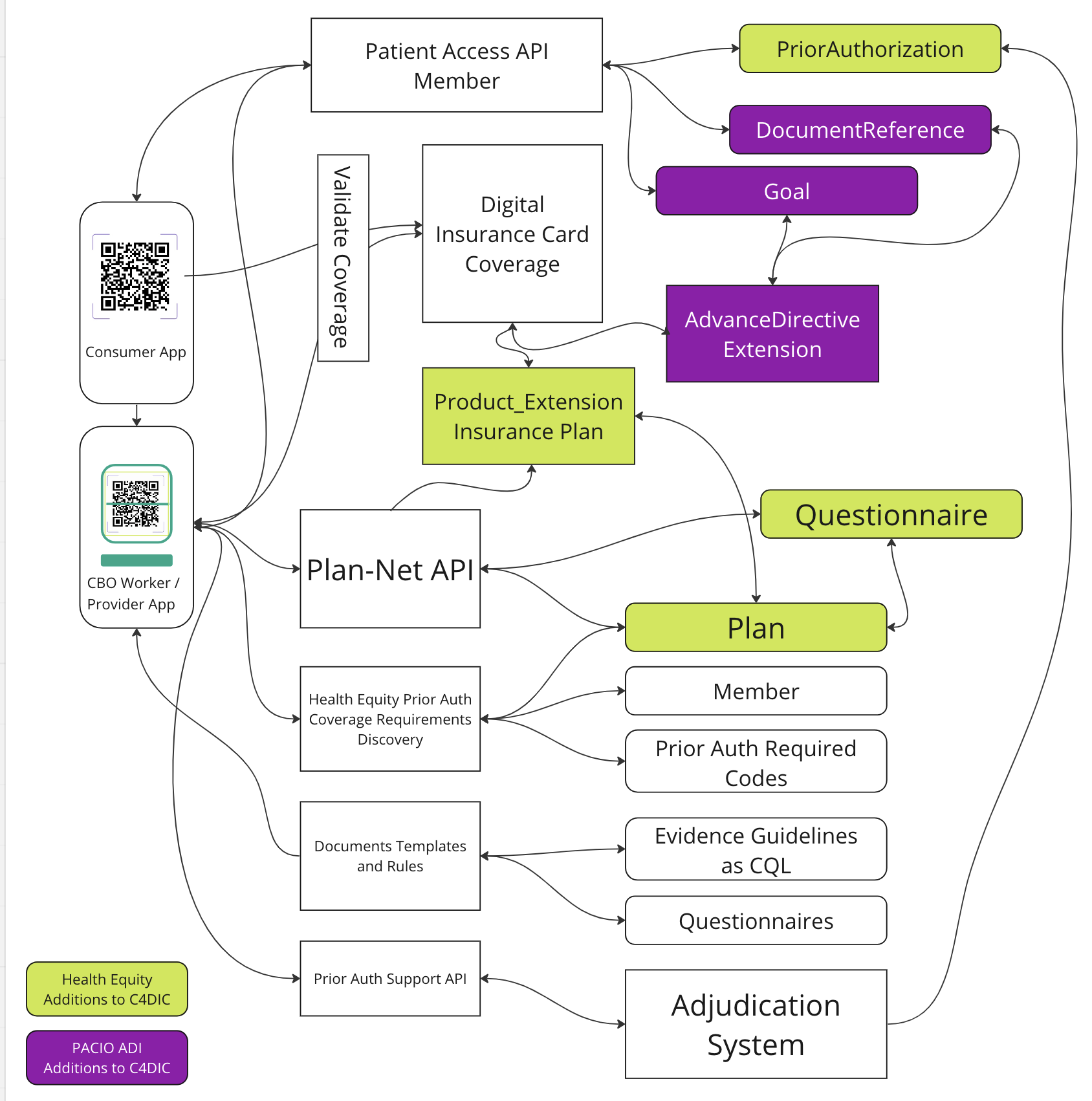
The illustration below shows the linkages between the different IGs.
Figure 1